The impact of long Covid on a person’s life can be devastating.
Opinion
Long Covid: the government needs to act now
The Office for National Statistics (ONS) estimates that one million people are living with long Covid across the UK, of whom 376,000 have been living with the condition for over a year.
It is a debilitating condition whose symptoms most commonly include extreme fatigue and shortness of breath, but it can affect any organ and can leave people unable to walk or work. Just under one in five (18.8 per cent) who suffer from the condition report that their daily lives have been limited a lot, according to the ONS.
 Layla Moran is Liberal Democrat MP for Oxford West & Abingdon
Layla Moran is Liberal Democrat MP for Oxford West & Abingdon
While men are more likely to die from Covid-19, long Covid disproportionately affects women of working age as well as those in keyworker roles, according to ONS analysis of population survey data on Covid-19. Keyworker status was defined by the government to include those in healthcare, social care, education, transport, food and agricultural services.
People in keyworker roles were required by government to go out to work during the pandemic to ensure that essential services could continue to operate, while the rest of society worked from home. Keyworkers were therefore at a greater exposure to the virus, as they were more likely to be in contact with other people in the performance of their jobs.
This increased risk is reflected in the recent studies of the prevalence of long Covid by the ONS. As of 6 March this year, 122,000 healthcare workers and 114,000 teachers were living with the condition. This is substantially higher proportionately than for other occupations in society. Indeed, the ONS studies suggest that those in health and social care are about twice as likely to have long Covid than the average worker.
The Industrial Injuries Advisory Council (IIAC) is currently reviewing the evidence on whether Covid-19 should be classified as an occupational disease as is already the case for healthcare workers in EU countries.
However, the general prevalence of Covid-19 in society makes establishing causation between occupation and infection more difficult. In such circumstances, in order to establish a direct link, the IIAC is looking to establish a two-fold risk at least from the workplace setting than exists in society as a whole.
While the ONS figures might suggest that that risk rate is established for certain occupations, the ONS states that it is not able to establish a straightforward cause-and-effect relationship between employment and Covid-19, because of the presence of other risk factors, such as age, pre-existing health conditions and the level of deprivation in the areas with increased prevalence of Covid-19.
As we wait for clarity, the impact of the condition continues to blight people’s lives. Freedom of Information requests to NHS trusts from the All-Party Parliamentary Group (APPG) on Coronavirus, which I chair, reveal that long Covid care is a postcode lottery.
Several long Covid clinics promised by government were not operating by the end of March, after government assertions that they were running in January, and there are areas of the country which still offer very little in terms of provision.
The APPG has received countless letters from people living with long Covid, who are unable to work and unable to access adequate support. They are now left with a long-term condition which affects not only their ability to return to work and live the healthy life that they had before the pandemic, but are also required to struggle without healthcare support and on inadequate sick pay protection schemes.
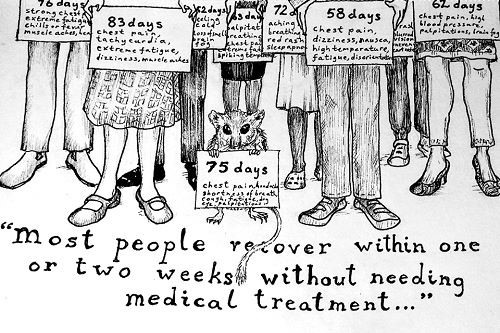 There is an urgent need for guidelines for employers and employees living with long Covid, to ensure that there is recognition of their symptoms. Illustration: LongCovid.org
There is an urgent need for guidelines for employers and employees living with long Covid, to ensure that there is recognition of their symptoms. Illustration: LongCovid.org
The APPG has twice written to the Prime Minister urging him to launch a compensation scheme for keyworkers who are struggling to return to work, and to class long Covid as an occupational disease. We continue to urge the UK government to count cases of long Covid and to publish the number of people living with the condition regularly.
We have urged the Prime Minister to improve the care for those living with long Covid and to increase research into the condition. Furthermore, we made clear that there is an urgent need for guidelines for employers and employees living with long Covid, to ensure that there is recognition, understanding and protection across all sectors of society.
Long Covid is a new condition. Employees and employers alike will be affected by long Covid and will undoubtedly need guidance to help them manage the condition in the workplace, particularly now that restrictions are being eased. Employees will need reassurance that they are protected, and that help is available.
It is of particular importance that this guidance recognises the condition’s long-term, relapsing and remitting nature. Employers will need guidance on the range of symptoms that can arise, the flexibility that may be required, and the need to ensure that employees do not feel that they are pressurised into coming back too early or for too many hours, as this can cause a relapse in symptoms.
This being a new condition is also why the government must urgently increase resources and funding for research, so that we can come to better understand and support those living with the condition which will remain as a lasting consequence of the pandemic for many years to come.
Long Covid is the hidden health crisis of the pandemic. Those living with the condition need protection and support from their employers, from the government and from the healthcare service. The government needs to accept its responsibility, acknowledge fully the sacrifices made and offer its unqualified support and protection, without further unnecessary delay.
For more information on the work of the APPG on coronavirus see:
appgcoronavirus.marchforchange.uk
And on long Covid, see here
Layla Moran is Liberal Democrat MP for Oxford West & Abingdon
OPINION

Violence against shop workers grows in an epidemic of retail crime
By Paddy Lillis, Usdaw on 26 April 2024
Violence against shop workers has more than doubled in a year, according to Usdaw’s latest annual survey, as official figures show that shoplifting has risen by over a third. Shoplifting is not a victimless crime; theft from shops has long been a major flashpoint for violence and abuse against shop workers.

ISO mental health standard needs a multi-disciplinary approach
By Phil Newton, Pinsent Masons LLP on 01 April 2022

Why your business should act on engine idling
By Jack Alexander, project officer, Idling Action London on 01 October 2021



