Many people will be affected by musculoskeletal problems during their working life, but there are simple steps employers can take to help them to remain in work, therefore retaining valuable members of staff.
Features
Backs for the future
The ‘musculoskeletal system’ is made up of over 200 bones in the skeleton, together with all the muscles, tendons and ligaments that join it all together and allow it to move.
These components together provide extraordinary strength to protect our vital organs (the heart, lungs and brain) but also facilitate fluid and fast mobility. The result is that humans can run 100 metres in under 10 seconds and walk away intact after a 200 miles per hour crash in a Formula 1 racing car.
However, to make this possible, there are many hundreds of separate moving parts throughout the system and this unfortunately provides opportunity for dysfunction and disorder.
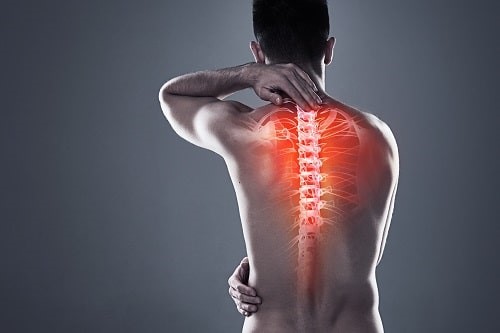 There are hundreds of moving parts in the musculoskeletal system, providing opportunity for dysfunction. Photograph: iStock / Peopleimages
There are hundreds of moving parts in the musculoskeletal system, providing opportunity for dysfunction. Photograph: iStock / Peopleimages
Therefore, the term ‘musculoskeletal disorders’ is an umbrella description for any condition or dysfunction impacting the musculoskeletal system. There are hundreds of common examples: arthritis; scoliosis; carpal tunnel syndrome; tennis elbow; bone fractures; a dislocated shoulder; sprained ankle; osteoporosis; fibromyalgia syndrome, to name just a few.
However, in practice, there are more common aches and pains affecting this system including – for example – back pain, neck pain, shoulder pain, knee pain etc. These aches and pains are part of normal everyday life, affect everybody at some point in time and for which there is often not a clearly identifiable pathology (there is pain but often no swelling or visible deformity or obvious structure that has ‘gone wrong’).
Such pains are probably part of normal human existence (back pain was written about in the old Egyptian papyrus), frequently come and go and generally do not need any medical input.
However, sometimes, they do not recover as expected and occasionally go on to cause chronic pain (pain lasting three months or longer); and this is often also associated with disability, depression, poorer quality of life and incapacity for work.
Some, but not all, of the reasons that pains become chronic have been identified. As a doctor specialising in musculoskeletal disorders, my role is to diagnose the conditions in which we understand the pathology in order to apply the best treatments (for example, a plaster cast for a broken bone; medications for arthritis). It is also my role to identify those at risk of chronic pain in order to try to maximise active recovery and prevent chronic pain and disability.
Why do musculoskeletal disorders matter at work?
During working life, when most people are ‘healthy’, they are still often affected by two types of problems: common mental health conditions like anxiety and depression and musculoskeletal disorders. Therefore, at any point in time, there will be a large number of workers (possibly as many as 30–40 per cent), who are currently experiencing some symptoms from one or other (or both) types of conditions.
 In many cases, people can (and will) come to work despite their symptoms of back pain. Photograph: iStock / simonkr
In many cases, people can (and will) come to work despite their symptoms of back pain. Photograph: iStock / simonkr
In many cases, people can (and will) come to work despite their symptoms, with a possible impact on their productivity but often without any change in their work performance. However, in some cases, the symptoms will be sufficiently severe that the worker will decide that they are not able to do their job and will self-certify their sickness or will seek a fit note from their GP.
Importantly, work (namely supportive, flexible work), can be part of the recovery from both these types of conditions (that is why phased returns to work are part of rehabilitation). Also, people do not need to be 100 per cent fit in order to attend work.
With musculoskeletal disorders, we know that prolonged sickness absence is particularly unhelpful and that the longer a worker stays away from their job, the less likely they are to ever return (less than 50 per cent of people off sick with back pain will ever return to work after six months’ sick leave).
Therefore, it is in the best interests of the employer and employee if the musculoskeletal symptoms can reasonably be accommodated while the individual continues to work (see the panel below). None of these measures are expensive or difficult and can usually be negotiated between the employee and their line manager – providing there is a culture of openness and supportive communication within the workplace.
If more expensive measures are needed, Access to Work is a government service specifically there to provide additional support and funding – see: www.gov.uk/access-to-work
Of course, any workplace accommodation might be temporarily inconvenient to the manager or team members or have adverse effects in the short term, but making such provisions pays off enormously in terms of loyalty, reduced staff turnover, reduced sickness absence and more readiness of team members to be open and honest and support each other and their manager.
Moreover, if the employee meets the very broad definition of being disabled as a consequence of their musculoskeletal disorder under the Equality Act, they are entitled to these types of ‘reasonable adjustments’ to enable them to participate in work equally to someone else without the disability.
What about chronic musculoskeletal disorders?
Even when a worker has a long-term musculoskeletal condition (such as arthritis), they can often remain at work. Some types of arthritis which were, in the past, very disabling (like rheumatoid arthritis, ankylosing spondylitis, psoriatic arthritis), have become much more treatable in the last 10–15 years. Once properly diagnosed, and treatment has been stabilised (which can sometimes take six to nine months), the employee may well be able to do their pre-diagnosis job as effectively as beforehand.
 The musculoskeletal system was designed to move and needs regular physical exercise and a well-balanced diet to retain its optimal performance. Photograph: iStock / TuiPhotoengineer
The musculoskeletal system was designed to move and needs regular physical exercise and a well-balanced diet to retain its optimal performance. Photograph: iStock / TuiPhotoengineer
The ideal type of line management during this phase would be supportive and accommodating, showing interest in what is going on (without requiring that the employee share confidential information), and supporting the individual through accommodation of their needs.
It includes enabling the individual to work if possible until a proper assessment is possible of how they are going to be affected in the long-term. Employers can ask the worker to obtain advice about working from either their GP or their specialist – providing that they do so sensitively and kindly and are doing so in the best interests of the worker, rather than the business.
Osteoarthritis is a very common type of arthritis which affects a very large number of people, particularly those aged over 50 years.
As we encourage people to remain working to older ages, we will see the numbers of people working despite this condition growing. Whilst there is no cure for osteoarthritis, it does not inevitably worsen over time and many patients do not need operations or medications.
However, osteoarthritis can cause pain and stiffness that fluctuate over time so that the symptoms are unpredictable and the pain often causes sleep disturbance. Most people with osteoarthritis can work very effectively but they may need to have flexibility to stand and stretch, to take a walk or breaks regularly, and may have occasional ‘bad days’ which require understanding and thoughtfulness.
Women are more prone to osteoarthritis than men and it may be that workforces with a female predominance – such as healthcare, social care and education – might need to consider the design of the work and the environment more carefully if they are to accommodate and retain growing numbers of older female workers.
What about when work causes musculoskeletal disorders or makes them worse?
As we have seen above, if work never caused musculoskeletal disorders, there would still be workers with musculoskeletal disorders who need to be accommodated in the workplace. However, unfortunately, some musculoskeletal disorders can be caused by work and many (if not all) can be made worse by work.
Of course, employers have a mandatory requirement, enforced by the Health and Safety Executive, to take reasonable steps to prevent harm to the health of their workers that might be caused by their work. This is where approaches such as manual handling risk assessments, employee training and the correct use of equipment are all an essential part of the employer’s responsibilities.
However, it is important to examine a few facts. Firstly, it is not only physical strains in the workplace that cause musculoskeletal disorders, or make them worse. While heavy lifting, working with abnormal postures, working outside and exposure to whole-body vibration all increase the risk of developing low back pain (by 15–20 per cent), so too does stress, excessive workload, poor job satisfaction, working at high pace, perceived low reward for considerable effort (each with magnitudes of effect similar to those reported for the physical factors). Therefore, ‘ticking the box’ for prevention of physical work strain will not prevent all work-related musculoskeletal disorders.
Secondly, it is either difficult or impossible to distinguish a musculoskeletal disorder caused by work from one not caused by work – back pain is back pain, whatever the cause. Clearly, if a worker fell off a high ladder at work because of negligence on the part of his employer, and has back pain now, he will quite rightly be able to attribute his pain to work and expect to be compensated for his injury and any resultant disability.
However, most musculoskeletal disorders amongst workers are not so clearly attributable and therefore, the best practice for employers would be to pay attention to provision of work that is flexible, well managed and supported with transparent communication so their employees do not perceive that they can blame their work for either causing their condition or making it worse.
How can we look after musculoskeletal health?
The musculoskeletal system was designed to move and needs regular physical exercise and a well-balanced diet to retain its optimal performance. Obesity is bad for the musculoskeletal system, not just because of mechanical factors (heavier strain through the load-bearing joints), but probably also through hormonal changes.
Muscle mass peaks at around 30 years of age, when it consolidates but slowly declines (even with regular exercise), from approximately age 40 years. It is for this reason that few professional athletes remain the fastest, strongest, and most competitive after their fifth decade of life (none of us expect Roger Federer to win Wimbledon again in his 50s).
Supporting employees to undertake regular physical exercise through incentivisation or providing workplace exercise facilities or gym memberships will therefore pay employers back, both in terms of improved job satisfaction but also in terms of improved musculoskeletal (and mental) health – facilitating greater physical resilience.
Conclusion
The musculoskeletal system is complex and sophisticated and consequently vulnerable. Most workers will experience one or more musculoskeletal disorders during their working lifetime. Employers should aim to create work environments that are flexible, supportive and accommodating and promote physical activity to workers, as these measures will enable the best chance of preventing work-related musculoskeletal disorders – and minimise sickness absence and maximise productivity.
Reasonable adjustments to enable accommodation of workers with musculoskeletal disorders
- Reducing or changing working hours or allowing flexibility of hours
- Rotation of tasks with co-workers
- Working from home
- Provision of tailored equipment (desk, chair, mouse, keyboard, voice-activated software)
- Car park space nearer to workplace
- Longer or more frequent breaks
- Provision of suitable space for stretching
- Time off to attend medical or rehabilitation appointments
- Re-locating to more accessible work space
- Reduction of physical loads
- Restriction of time spent doing repetitive tasks
- Provision of flexible working
- Re-deployment to a more suitable role
- Providing support for travel to/from work.
The above content is adapted from: www.councilforworkandhealth.org.uk/work-modifications
About the author
Karen Walker-Bone is director of the MRC Versus Arthritis Centre for Musculoskeletal Health and Work and Professor of Occupational Rheumatology at the University of Southampton.
Contact her at: [email protected]
FEATURES

Backstage pass: how do festival organisers keep staff and visitors safe?
By Kerry Reals on 29 April 2024
As festivalgoers prepare to pull on their wellies, dig out their sunhats and dust off their tents ahead of another summer of live outdoor events, Safety Management looks behind the scenes at how festival organisers keep the armies of workers tasked with setting everything up safe and well.

AI: a powerful new tool for managing safety risks
By Robert Leech, EcoOnline on 29 April 2024
AI-driven technology is revolutionising the management of occupational safety and health, making it easier to spot hazards, predict unsafe behaviours and take preventative action to protect workers.

Pursuing workplace wellbeing through authentic leadership
By Dr Audrey Fleming, British Safety Council on 26 April 2024
By being open, honest and vulnerable in their interactions at work – and genuinely seeking and valuing the input of employees – leaders can develop a workplace atmosphere where trust and respect flourish, in turn supporting the wellbeing, engagement and performance of their teams.



